












The binocular slit-lamp examination provides a stereoscopic magnified view of the eye structures in detail, enabling anatomical diagnoses to be made for a variety of eye conditions. A second, hand-held lens is used to examine the retina. A slit-lamp exam is usually done during a regular checkup with your eye doctor before the cataract surgery procedure.
A Keratometer, also known as an ophthalmometer, is a diagnostic instrument for measuring the curvature of the anterior surface of the cornea, which is used to assess the amount and axis of astigmatism. Keratometry is the measurement of the corneal curvature determining the power of the cornea.
A pachymeter is a medical device used by the doctor to do a test called pachymetry. It is a simple, quick, painless test to measure the thickness of your cornea. With this measurement, your doctor can better understand your IOP reading, and develop a treatment plan that is right for your condition. The procedure takes only about few minutes to measure both eyes.
It is used to monitor and measure changes that may occur to the shape and integrity of the cornea of your eye. A corneal topographer projects a series of illuminated rings, referred to as a Placido disc, onto the surface of the cornea. The rings are reflected back into the instrument.
.
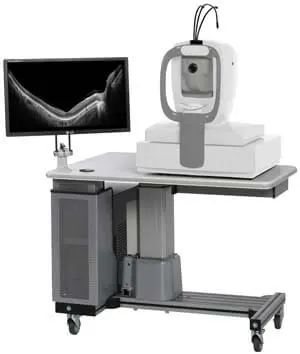
Optical coherence tomography (OCT) is a noncontact technology that produces high-resolution cross-sectional images of ocular tissues. Anterior segment OCT (AS-OCT) enables the precise visualization of anterior segment structure; thus, it can be used in various corneal and ocular surface disorders.
Corneal Collagen Cross-Linking with Riboflavin (also abbreviated as C3R) is a non-invasive corneal treatment shown to slow the progression of keratoconus. It does so by increasing the strength of corneal tissue. Undergoing C3R in the early stages may help stabilize vision.





The central portion of the eye in the front is a clear glass like structure (appears black/brown due to underlying tissues) is known as the cornea. Any white appearance/spot on the cornea is abnormal and can result in blindness. It could be due to an infection (ulcer), traumatic scar, age-related degeneration, dystrophy (genetically acquired) or swelling (edema). Treatment prescribed by your ophthalmologist may be medical or surgical, based on the etiology.
Computer vision syndrome or digital eyestrain is a condition that occurs due to looking at computer/mobile or other screens for long periods of time. This occurs due to inability of eye muscles to recover from the strain caused by constant focusing on a near target, and may result in dry eyes. Taking regular breaks (at least for 20 seconds every 20 minutes), placing the monitor at least 25 inches away from eye, reducing monitor brightness, using anti-glare spectacles, blinking frequently and using lubricating eye drops help in reducing symptoms.
Viruses or bacteria can cause an infection of the superficial structures of the eye; characterized by redness, watering, and/or defective vision. This is known as conjunctivitis or popularly as Madras eye. The condition usually takes 2-6 weeks to resolve and may be transmitted from one person to another through contact in the initial 1-2 weeks. Using the correct eye medication and hand hygiene ensures appropriate treatment of this condition.
A cornea transplant is an operation to remove all or part of a damaged cornea and replace it with healthy donor tissue. A cornea transplant is often referred to as keratoplasty or a corneal graft. It can be used to improve sight, relieve pain and treat severe infection or damage.
Eyes can be donated after death (ideally within 6 hours) by any individual irrespective of age. The cornea and sclera harvested from the donated eye is utilized for transplantation surgery. In no case, is the donation wasted. The only contraindications for utilization for surgery are the presence of certain types of cancers and certain types of infections in the donor, that hold the risk of transmission to the recipient; however they can be utilized for training and research.
A non-seeing blind eye that cannot be visually rehabilitated often may require a cosmetic correction; due to presence of white discoloration, protrusion and squinting. A colored contact lens, corneal tattooing with a black/brown pigment, squint surgery and evisceration with implantation of a prosthetic eye are the available options.
Contact lenses are thin transparent devices that can correct the eye power. They are placed directly on top of the cornea. Regular cleansing of lenses before and after use, restricting usage to 8-9 hours/day, avoiding overnight use, regular replacement and avoiding dust/water from directly touching the lens; are some practices for good hygiene. Immediately remove your contact lenses if you develop redness or pain while wearing them and consult your ophthalmologist.
Keratoconus is a condition characterized by progressive protrusion and thinning of the cornea, which can lead to poor vision, visual distortions, and/or whitening of the cornea. The various treatment options available are spectacles, contact lenses, crosslinking (corneal strengthening), intracorneal rings, laser vision correction with crosslinking, and implantable Collamer lenses. Early recognition and management are the keys to a successful outcome.
1, Tapovan Society Nr. Nehrunagar Cross Road Satellite, Ahmedabad, Gujarat - 380015 | TEL: +91 7926753534
Opp. Z. K. Hotel Relief Road, Ahmedabad, Gujarat - 380001 | TEL: +91 7925506257
307-311, Iconic Isanpur, Near Honda showroom, Next to Indian Oil Petrol Pump, Naroda Narol Highway, Isanpur, Ahmedabad, Gujarat - 382443 | TEL: +91 9979393783
102,103, B Square 2, Vikram Nagar, Iscon-Ambli-Bopal Road, Ahmedabad, Gujarat - 380054 | TEL: +91 8160755086